Exploring the Crucial Role of Temperature Measurement in South Africa's Healthcare System
Understanding the Critical Nature of Effective Temperature Monitoring for Health
Monitoring body temperature is a fundamental aspect of healthcare, particularly within the diverse climate of <a href="https://limitsofstrategy.com/goose-valley-golf-club-the-top-golf-course-in-south-africa/">South Africa</a>. The country boasts a wide range of climatic conditions, from the warm coastal areas to the chillier highlands, making accurate temperature measurements essential. Elevated body temperatures can often indicate serious health concerns, such as infections, necessitating immediate medical intervention. Given the rich diversity of South Africa's population along with its unique ecological zones, precise temperature monitoring is crucial. For example, in regions with significant altitude variations like the Drakensberg, baseline temperatures may differ due to environmental influences. This variability can profoundly affect health assessments and treatment approaches, highlighting the importance of mastering accurate temperature measurement techniques and their interpretation for effective health management across diverse demographic groups.
Evaluating Common Temperature Measurement Methods in South Africa
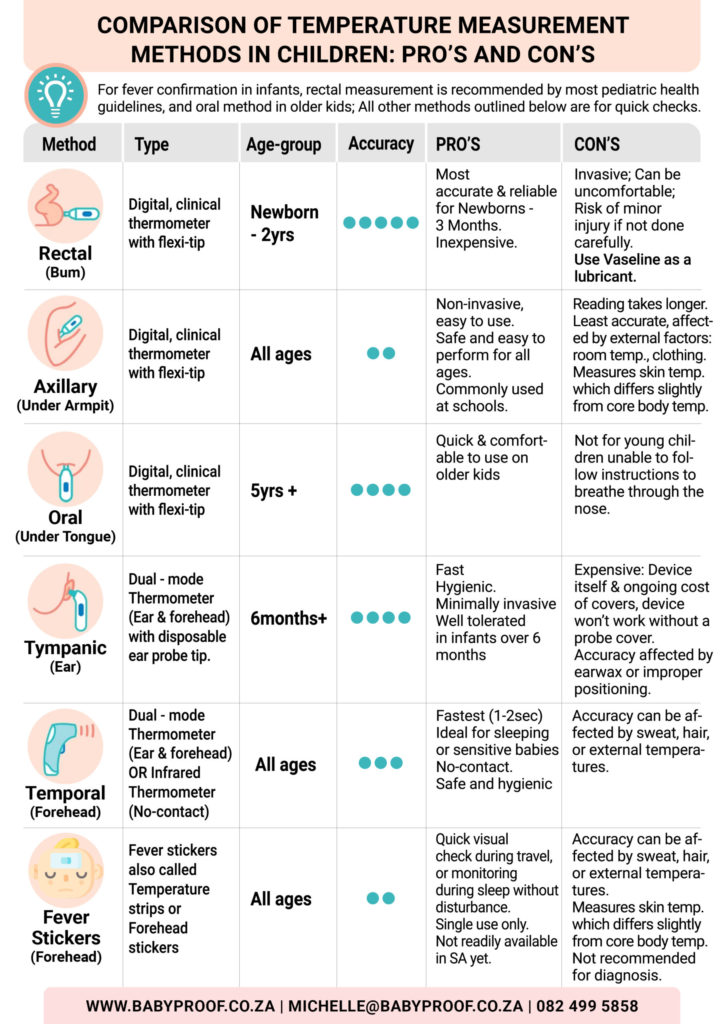
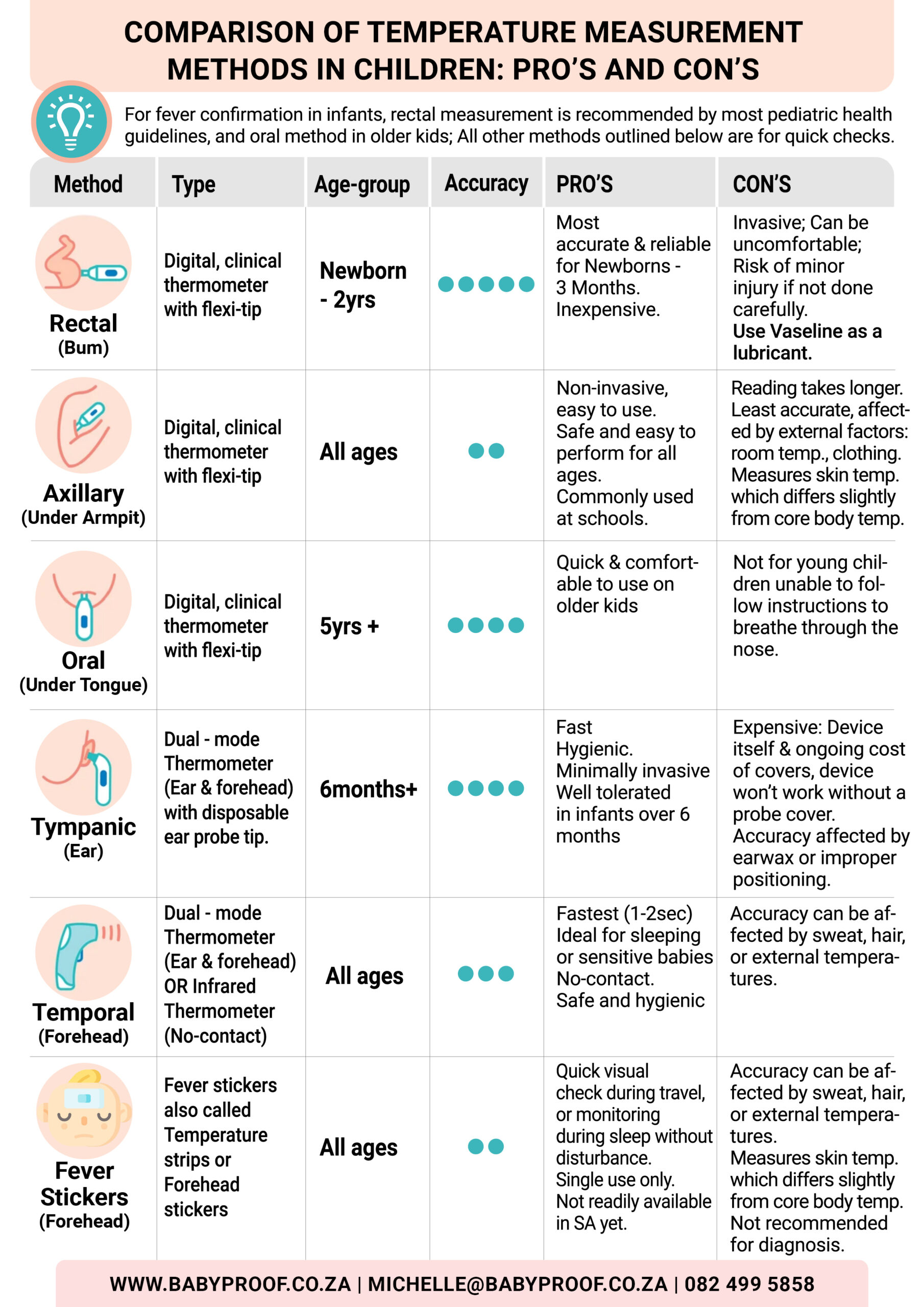
In South Africa, the commonly used methods for measuring body temperature include oral, axillary, and rectal techniques, each with unique advantages and practical applications tailored to specific circumstances. Oral thermometers are widely available in households and clinics, offering a convenient and reliable option for measuring temperature. While axillary measurements are often employed in schools and childcare settings due to their non-invasive nature, they are typically acknowledged as less accurate. On the other hand, rectal measurements, though less frequently used outside clinical settings, are considered the gold standard for precision, particularly for vulnerable populations like infants or critically ill patients. A thorough understanding of these methods and their appropriate applications is essential for effective health monitoring across South Africa.
Tailoring Temperature Measurement Techniques to Different Age Groups
- Newborn – 3 months → Utilise Rectal (the most reliable) or Temporal (forehead) for rapid screening.
- 3 months – 3 years → Rectal for precision; Temporal (forehead) or Axillary (underarm) for comfort.
- 4 – 5 years → Oral if the child can cooperate; Temporal (forehead), Tympanic (ear), Axillary (underarm) for quick checks. Fever Stickers may also be considered.
- 6+ years → Oral is recommended for the best balance of accuracy and comfort; Temporal (forehead) or Tympanic (ear) for swift assessments.
The Vital Importance of Accurate Temperature Readings for Positive Health Outcomes
Accurate temperature readings are essential for diagnosing illnesses and monitoring health, particularly in South Africa, where diverse environmental conditions can have a significant impact on physiological responses. In clinical contexts, healthcare professionals rely on precise temperature measurements to make informed decisions regarding treatment protocols. For instance, an inaccurately recorded temperature may lead to unnecessary treatments or delayed interventions for serious medical conditions. Moreover, in public health initiatives, ensuring accurate temperature readings significantly enhances the effectiveness of health responses, especially during outbreaks of infectious diseases. Therefore, the vital role of accuracy in temperature measurement cannot be overstated, as it directly affects patient outcomes and overall public health.
Recognising the Impact of Altitude on Temperature Measurement Accuracy
South Africa's varying altitudes present unique challenges for accurate temperature measurement. Locations such as Johannesburg, situated around 1,753 meters above sea level, may experience temperature reading fluctuations compared to coastal cities like Durban. Increased altitude can alter body metabolism and thermoregulation, thus necessitating careful adjustments when interpreting temperature readings. Healthcare providers must take these variations into account when assessing patients from diverse regions. For instance, a fever in a patient from a high-altitude area may present differently than in someone from a lower elevation. Acknowledging these nuances is crucial for accurate health assessments and tailored patient care.
Advancements in Temperature Monitoring Technology: A Modern Approach
In recent years, South Africa has experienced considerable technological advancements that enhance the efficiency and accuracy of temperature monitoring. Innovations such as infrared thermometers and digital devices are gaining popularity in both clinical and home environments. These modern devices offer rapid readings and frequently incorporate user-friendly features, including backlit displays and memory functions. Additionally, smartphone-connected thermometers are becoming increasingly popular, enabling users to track temperature readings over time and easily share this information with healthcare providers. These advancements in technology streamline the temperature measurement process and hold the potential to improve health outcomes by facilitating timely medical interventions.
Mastering the Techniques of Oral Temperature Measurement in South Africa
Expert Guidance on Taking an Accurate Oral Temperature Reading
Obtaining an oral temperature reading is a straightforward procedure requiring the thermometer to be placed under the tongue while ensuring the mouth remains closed for an accurate measurement. Before taking the reading, it is essential to confirm that the patient has not consumed hot or cold foods or beverages for at least 15 minutes, as these can significantly alter the results. Once the thermometer is positioned correctly, wait for the device to indicate that the reading is complete, typically accompanied by a beep. It is vital to educate patients and caregivers on this technique to ensure it is performed accurately, thereby avoiding misleading readings. This method is commonly employed in South African households, providing a convenient way for family members to monitor their health.
The Benefits of Oral Temperature Measurement in Daily Use
Oral temperature measurement offers a range of advantages that make it a preferred option in numerous South African homes and healthcare settings. Firstly, this method is non-invasive, significantly reducing discomfort often associated with alternative temperature-taking techniques. Secondly, it is user-friendly, enabling individuals to take readings without needing professional assistance. This convenience makes it particularly suitable for quick checks at home, allowing families to easily monitor fevers in both children and adults. Additionally, oral thermometers generally provide rapid results, typically within one to two minutes, facilitating prompt health decisions. In the fast-paced environments found throughout South Africa, this efficiency is particularly beneficial.
Recognising the Limitations and Considerations of Oral Temperature Measurement
While oral temperature measurement boasts several benefits, it is not devoid of limitations. This method may not be suitable for all patient demographics, particularly young children or individuals unable to keep the thermometer in place for the required duration. Moreover, factors such as recent food or drink consumption, smoking, or even breathing through the mouth can compromise the accuracy of readings. In South Africa, where environmental conditions can differ significantly, outdoor temperatures may also influence results if the thermometer is not used correctly. Thus, when employing the oral method, it is crucial to consider these factors to achieve the most accurate results possible.
Examining Axillary Temperature Measurement Techniques in South Africa
Proper Methodology for Measuring Temperature Using the Axillary Technique
The axillary method involves placing the thermometer in the armpit while ensuring that the arm is pressed snugly against the body to obtain an accurate reading. This technique is widely utilised in South African schools and childcare settings due to its safety and ease of implementation for all age groups. Ensuring that the skin is dry and that the thermometer is correctly positioned is essential for optimal accuracy. Although the reading may take longer than oral methods, often requiring several minutes, educating caregivers and staff on proper technique is vital to ensure that temperature readings are reliable and effective for identifying health issues in both children and adults.
Advantages of the Axillary Temperature Measurement Method in Public Health
Axillary temperature measurement presents numerous benefits, particularly in public health settings throughout South Africa. One of the primary advantages is its non-invasive nature, making it safe for individuals of all ages, including infants and the elderly. The simplicity of this method allows for quick execution in school health programmes or health fairs, where time constraints may be prevalent. Additionally, the axillary approach is cost-effective, requiring fewer resources compared to advanced digital or infrared thermometers. This accessibility is especially vital in rural areas, where healthcare resources may be limited. The straightforwardness and safety of axillary measurements make them an excellent option for community health initiatives.
Factors That Affect the Accuracy of Axillary Temperature Measurements
Despite its advantages, several factors can influence the accuracy of temperature readings obtained through the axillary method. Environmental conditions, such as high ambient temperatures or humidity prevalent in South Africa, may lead to elevated readings due to perspiration, potentially indicating a false fever. Furthermore, clothing can create insulation, hindering heat exchange and distorting results. Movement during the measurement process, particularly in children, can also lead to inaccuracies. Therefore, healthcare providers and caregivers must be aware of these factors and take measures to mitigate their impact, such as ensuring the arm remains close to the body and that the skin is dry prior to taking measurements.
Understanding Rectal Temperature Measurement Techniques in South Africa
Step-by-Step Guide to Accurately Measuring Rectal Temperature
Accurately measuring rectal temperature involves several steps to ensure both precision and patient comfort. Firstly, it is essential to apply a lubricating gel to the tip of the thermometer to facilitate gentle insertion. The thermometer should be inserted approximately an inch into the rectum while being held securely, waiting for the reading to complete. This method is frequently employed in South African hospitals due to its precision, particularly in critical care situations or when monitoring infants. Given the sensitivity of this method, performing the process gently and with the patient's comfort in mind is crucial for maintaining trust and cooperation from patients, especially vulnerable individuals.
The Rationale Behind Rectal Temperature Measurement as the Most Accurate Method
Rectal temperature measurements are widely regarded as the most accurate compared to oral and axillary methods, making them ideal for critical care situations in South Africa. This accuracy is particularly essential in emergency contexts or when dealing with unresponsive patients, as healthcare professionals rely on precise temperature information to inform treatment decisions. Additionally, rectal thermometers are less susceptible to external factors, such as ambient temperature fluctuations or recent oral intake, rendering them a reliable choice in clinical practice. In pediatric care, especially for infants, rectal measurements provide an authoritative assessment of core body temperature, enabling timely and appropriate medical interventions.
Essential Considerations and Precautions for Using the Rectal Method
While the rectal measurement method offers several advantages, it necessitates specific considerations and precautions. The insertion process can be uncomfortable, potentially leading to patient resistance, particularly in non-clinical environments. Therefore, it is vital to clearly explain the procedure and reassure the patient to foster cooperation. Furthermore, healthcare providers must adhere to strict hygiene protocols to prevent any potential infections or injuries. Due to these concerns, rectal measurements are less frequently performed in home settings across South Africa. Nevertheless, understanding when and how to employ this method is critical for healthcare professionals to ensure the utmost care and accuracy in temperature monitoring.
Expert Guidelines for Selecting the Best Temperature Measurement Method
Recommendations from South African Health Experts on Temperature Measurement
Healthcare professionals in South Africa typically recommend various temperature measurement methods based on multiple factors, including the patient's age, health condition, and specific context. For instance, oral measurements are often suggested for adults and older children who can securely hold the thermometer. Conversely, axillary readings might be preferred for quick assessments in schools or community health screenings. Rectal measurements are generally advised for infants or critically ill patients due to their accuracy. Below are some expert recommendations:
- For adults: Prefer oral or rectal readings for enhanced accuracy.
- For young children: Use axillary or rectal methods based on cooperation levels.
- For infants: Rectal measurements are the gold standard for precision.
- In school settings: Axillary readings are often sufficient for quick health checks.
- In emergencies: Prioritise rectal measurements for accurate assessments.
These recommendations underscore the importance of selecting the temperature measurement method tailored to the individual needs of each patient and the context in which care is provided.
Impact of Environmental Conditions in South Africa on Temperature Readings
Environmental factors in South Africa significantly affect temperature readings, necessitating that healthcare providers consider context while interpreting data. For instance, in coastal areas where humidity levels are high, axillary temperature readings may be artificially elevated due to excessive sweating, potentially leading to misdiagnosis. Similarly, in colder regions, such as the Drakensberg, ambient temperatures can cause a drop in readings, prompting healthcare professionals to remain vigilant about local conditions. Experts advocate that practitioners adjust their interpretation of temperature data based on these environmental variables, ensuring accurate assessments. This contextual awareness is essential for appropriate diagnosis and treatment.
Implementing Best Practices for Temperature Measurement in South Africa
Implementing best practices for temperature measurement is crucial in South Africa to ensure accurate and reliable readings. These practices include regularly calibrating thermometers to maintain their precision, as poorly calibrated devices can yield misleading results. Moreover, healthcare providers should consider patient conditions and adapt their temperature measurement techniques accordingly. For instance, taking into account a patient’s hydration status can significantly influence readings. Providers should also educate patients and caregivers about the importance of using proper measurement techniques, including the best times to take readings and understanding factors that may affect temperature. By adhering to these best practices, healthcare professionals can significantly improve the quality of care provided.
Cultural Influences on Temperature Measurement Preferences in South Africa
Cultural beliefs significantly shape temperature measurement preferences in South Africa. Various communities may favour specific methods based on traditional practices or comfort levels. For instance, some cultures might prefer non-invasive methods like axillary measurements due to a preference for less intrusive techniques. Recognising these cultural nuances is vital for healthcare providers to deliver culturally sensitive care. Engaging with communities to educate them about the benefits and limitations of each temperature measurement method can build trust and improve adherence to recommended practices. Furthermore, respecting cultural beliefs while offering evidence-based recommendations can enhance patient cooperation and health outcomes.
Challenges Faced in Implementing Diverse Temperature Measurement Methods in South African Health Facilities
Implementing temperature measurement methods in South African health facilities presents a variety of challenges, including resource availability and staff training. In rural areas, healthcare facilities may lack access to modern temperature-taking devices, which can limit effective monitoring. Additionally, staff may require continuous education and training to ensure proficiency in accurately using various measurement methods. High patient volumes in urban clinics can also lead to time constraints, resulting in rushed assessments and potential inaccuracies. Addressing these challenges through targeted training programmes and improved access to equipment is essential for enhancing temperature monitoring practices throughout South Africa's diverse healthcare landscape.
Comparative Insights into Oral, Axillary, and Rectal Temperature Measurement Methods
Key Differences Between Temperature Measurement Approaches
The primary distinctions among oral, axillary, and rectal temperature measurement methods revolve around accuracy, ease of use, and appropriateness for different age groups and settings. Oral thermometers provide reliable readings and are commonly utilised for adults and older children; however, they require patient cooperation, which may not always be attainable. Axillary temperature measurements are non-invasive and suitable for all ages, making them ideal for community screenings; however, they tend to be less precise. Rectal measurements, often regarded as the most accurate, can cause discomfort and may not be suitable for all patients outside clinical environments. Understanding these differences is crucial for selecting the most appropriate method for each situation.
Assessing Accuracy and Reliability Across Various Measurement Methods
In South Africa, the accuracy and reliability of temperature readings vary across different methods. Rectal measurements are generally acknowledged as the most accurate, closely reflecting core body temperature. Oral measurements follow, providing reliable readings when performed correctly, while axillary measurements typically yield the least accurate outcomes. This hierarchy of accuracy guides healthcare providers in their decisions, especially when assessing febrile patients or making critical care choices. For example, in emergency situations, rectal readings may be prioritised to ensure precise monitoring of patients' conditions. Recognising the limitations of each method can significantly enhance the quality of healthcare in South Africa.
Evaluating the Suitability of Each Temperature Measurement Method in South African Contexts
The appropriateness of each temperature measurement method within South African contexts hinges on various factors, such as the setting and the patient's specific needs. In home environments, oral measurements are often preferred for older children and adults due to their convenience. Conversely, axillary measurements may be standard in schools or during community health campaigns, where quick assessments are necessary. Rectal measurements, while ideal for precise monitoring in clinical settings, may be less suitable for home use due to comfort concerns. Therefore, healthcare providers must carefully assess each situation, considering available resources and the patient's condition to determine the most suitable temperature measurement method.
Practical Considerations for Effective Temperature Measurement in South Africa
Available Equipment and Resources for Temperature Measurement Across South Africa
The array of equipment and resources for temperature measurement in South Africa varies significantly. From basic digital thermometers to advanced clinical devices, there is an extensive range of options available. In urban hospitals, cutting-edge technology is frequently employed, including infrared thermometers, which enable rapid and contactless measurements. Conversely, in rural settings, basic thermometers may be the only available option, potentially impacting the accuracy of readings. The availability and affordability of these tools greatly influence healthcare practitioners’ choice of methodologies throughout the country. Ensuring that healthcare facilities, particularly in underserved areas, have access to reliable equipment is essential for effective patient care.
Challenges Encountered in Temperature Measurement Practices
Healthcare providers in South Africa face numerous challenges regarding temperature measurement. Limited resources, especially in rural regions, can restrict access to accurate and reliable thermometers. Furthermore, patient cooperation can be unpredictable, particularly in children or individuals with cognitive impairments, complicating accurate measurement. Unique environmental factors, such as extreme heat or cold, can also interfere with readings and complicate assessments. Overcoming these challenges necessitates employing strategies like community education initiatives, enhancing equipment access, and training healthcare providers on best practices for temperature measurement.
Strategies to Ensure Accurate Temperature Readings in South Africa
Achieving accurate temperature readings in South Africa involves several critical steps. Firstly, healthcare providers should consistently evaluate their techniques to ensure adherence to best practices for each measurement method. Regular calibration of thermometers is also essential to maintain accuracy. Educating patients and caregivers about the significance of proper technique, including factors that can affect readings, such as recent food intake or environmental temperature, can greatly enhance assessment reliability. Practitioners should also consider the distinct environmental conditions of South Africa to appropriately adjust their interpretation of readings, thereby ensuring comprehensive patient care.
Proven Strategies for Selecting the Optimal Temperature Measurement Method
Guidelines for South Africans on Choosing the Most Effective Method
Selecting the best method for temperature measurement in South Africa requires thoughtful consideration of several factors. Firstly, the patient's age and health condition significantly influence the appropriate method. For example, infants may necessitate rectal measurements for accuracy, while older children might be more suited to oral or axillary methods. Additionally, the setting—whether in a clinical environment, at home, or during a community health event—should guide the choice of measurement. South Africans can adopt these strategies to ensure informed decision-making:
- Assess the patient’s age and level of cooperation.
- Consider the urgency of the temperature assessment.
- Evaluate available equipment and resources.
- Be aware of environmental conditions that may affect readings.
By following these steps, individuals can ensure they select a method that delivers reliable results.
Best Practices for Each Temperature Measurement Method in South Africa
Implementing best practices for temperature measurement is critical across all methods used in South Africa. For oral measurements, always confirm that the patient has not consumed anything that could affect readings beforehand. When performing axillary measurements, keeping the arm close to the body and ensuring the skin is dry will yield better accuracy. Rectal measurements require careful handling and clear communication with the patient to minimise discomfort. Best practices for each method include:
- Regularly calibrate thermometers to ensure accurate readings.
- Educate patients and caregivers on proper techniques.
- Consider environmental factors when interpreting results.
- Document findings accurately to facilitate ongoing health assessments.
Following these practices will enhance the reliability of temperature measurements and improve health outcomes throughout South Africa.
Strategies for Public Education on Temperature Measurement
Public education regarding temperature measurement is essential for enhancing health literacy across South Africa. Healthcare providers can establish clear guidelines outlining the importance of accurate temperature readings and how to measure them effectively. Community outreach programmes, workshops, and health fairs can serve as platforms to educate the public about various temperature measurement methods. Moreover, utilising local healthcare resources, such as clinics and hospitals, to disseminate information and provide demonstrations can improve understanding. By focusing on practical application and cultural relevance, healthcare professionals can foster a more informed public capable of effectively monitoring their health.
Assessing the Best Temperature Measurement Method in South Africa
Key Insights on Temperature Measurement Practices
Oral, axillary, and rectal temperature measurement methods each possess distinct advantages and limitations within South African healthcare. Understanding the unique characteristics of each method, including accuracy, ease of use, and age appropriateness, is crucial for effective health monitoring. By being aware of the environmental factors that can influence readings, healthcare professionals can make informed decisions that enhance patient care.
Guidelines for Healthcare Providers in South Africa
Healthcare providers in South Africa should consider individual patient needs, including age and health status, when selecting temperature measurement methods. Furthermore, they should remain cognizant of available resources and the environmental context to ensure accurate assessments. Ongoing training and education on the latest best practices will further empower providers to deliver high-quality care in temperature monitoring.
Emerging Trends in Temperature Measurement Within South Africa
Future trends in temperature measurement may include the adoption of advanced technologies, such as smart thermometers that connect to mobile applications for tracking health metrics. Enhanced public education initiatives can further elevate health literacy regarding temperature measurement. Additionally, tailored approaches that consider South Africa's unique cultural and environmental contexts will improve the effectiveness of healthcare delivery in temperature monitoring.
Disparities in Temperature Measurement Between Rural and Urban Settings
The choice of temperature measurement methods can differ dramatically between rural and urban settings in South Africa. Limited access to advanced equipment in rural areas may necessitate reliance on simpler methods like axillary readings. In contrast, urban facilities typically have access to a wider array of technological options, permitting more precise measurements. Addressing these disparities through targeted resource allocation and training is vital to ensure equitable healthcare access.
The Impact of Cultural Practices on Temperature Measurement Preferences
Cultural beliefs and practices significantly shape attitudes towards temperature measurement methods in South Africa. Understanding and respecting these beliefs is imperative for healthcare providers to deliver culturally sensitive care. By engaging with community leaders and incorporating culturally relevant practices into health education, providers can ensure that temperature measurement methods are accepted and effectively utilised within various cultural contexts.
Frequently Asked Questions Regarding Temperature Measurement
Which method is the most accurate for measuring body temperature?
The rectal method is widely regarded as the most accurate for measuring body temperature, as it closely reflects core body temperature and is less influenced by external factors.
Can axillary temperature be relied upon for accurate diagnosis?
While axillary temperature is non-invasive and safe, it is generally less accurate than oral or rectal methods. However, it can still provide useful information in non-critical settings.
What is the proper technique for taking an oral temperature reading?
To take an oral temperature, place the thermometer under the tongue, close the mouth, and wait for it to beep. Ensure that no hot or cold food or drink has been consumed beforehand.
What factors can affect the accuracy of axillary temperature readings?
Factors such as ambient temperature, humidity, clothing, perspiration, and movement can all influence the accuracy of axillary temperature readings.
Is it safe to measure rectal temperature at home?
While rectal measurements are accurate, they can be uncomfortable. They are generally recommended for infants or in clinical settings rather than at home unless advised by a healthcare professional.
What technology is available for temperature measurement in South Africa?
In South Africa, a variety of technologies is available, ranging from basic digital thermometers to advanced infrared devices that enable quick, non-contact temperature measurements.
How often should thermometers undergo calibration?
Thermometers should be calibrated regularly to ensure accuracy, ideally before significant use each season or at least once a year.
What steps should I take if my temperature reading is abnormal?
If a temperature reading is abnormal, especially if accompanied by other symptoms, it is advisable to seek medical advice for further evaluation and potential treatment.
Are there cultural preferences for temperature measurement methods in South Africa?
Yes, cultural beliefs can impact preferences for specific temperature measurement methods. Understanding these beliefs is vital for providing culturally sensitive healthcare.
How can I learn more about temperature measurement techniques?
You can learn more about temperature measurement techniques through local healthcare providers, community health workshops, and online resources dedicated to health education.
Explore our updates on Instagram!
The article Best Method for Temperature: Oral, Axillary, or Rectal? A South African Guide was published first on: https://www.babyproof.co.za
The Article Temperature Measurement Methods: Oral, Axillary, or Rectal? Was Found On https://limitsofstrategy.com